


Adverse Event reporting information can be found in footer
Request a Meeting
The burden of PNE on children and their families is considerable5.
PNE can be a persistent problem, and 10% of enuretic children will remain bedwetters for life1.
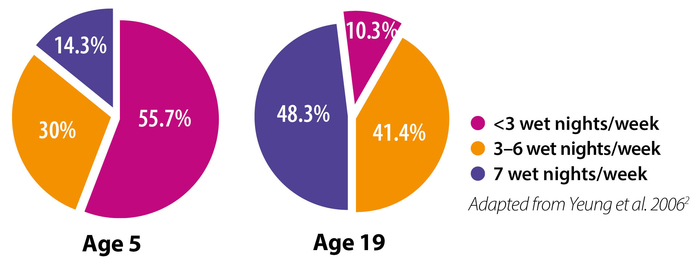
Enuretic symptoms in adolescent subjects were more severe than those in children2. This shows early intervention
can be key in PNE.
Most cases of PNE have two main causes:
This is the most common cause of bedwetting. Most bedwetting children are delayed in developing the ability to stay dry and have no other developmental issues2,6. Bedwetting may be due to a nervous system that is slow to process the feeling of a full bladder1,7.
Bedwetting has a strong genetic component. Children whose parents were not enuretic have a 15% incidence of bedwetting. However, when one or both parents were enuretic, the rates jump to 44% and 77% respectively8.

Due to low vasopressin levels, and subsequently, a reduced or absent nightly spike in vasopressin concentration which normally keeps bladder volume from reaching capacity until morning1,9
If the child does not wake at the feeling of a full bladder, the child will more likely wet the bed1,9
The muscles of the bladder can suddenly contract before the bladder is full9
Nocturnal enuresis (NE) is also linked to one (or a combination) of the following factors: anxiety, stress, small bladder size, constipation, and urinary tract infection7
The burden of PNE on children and their families is significant5; however, effective treatment benefits all parties6.
Job Code: UK-MN-2200029 - Date of preparation: March 2023